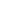Adjusting to life with respiratory challenges or a ventilator can seem overwhelming, but understanding the available resources makes living with a ventilator manageable. Our respiratory therapy and ventilator program is designed to give patients the best achievable quality of life.
Respiratory therapy at Hillcrest Commons features:
- Dedicated ventilator unit led by board-certified pulmonologist
- Focus on increasing mobility and weaning dependence whenever possible
- 24-hour respiratory therapists
- Regular consultations with Berkshire Medical Center pulmonologists
- Nurse practitioner hospitalist on unit daily for medical interventions
- Speech therapy for bedside swallow evaluations and communication strategies
- Physical and occupational therapy to increase endurance and ability
What does a ventilator mean for me or my loved one?
While the terms “pulmonary” and “respiratory” are generally used to describe breathing and the lungs, our program takes respiratory care to another level. We’ve learned never to underestimate our patients, as many individuals with tracheostomies or ventilators can live independent, active lives. As one patient put it, “I’m not attached to the ventilator. The ventilator is attached to me.” Life with a ventilator can bring unique challenges, but the right care can help you gain strength and confidence.
Ventilators may sound scary, but they are specialized equipment commonly used to facilitate breathing following illness or injury. A tracheostomy, or “trach” (rhymes with “rake”) is a surgically created opening in the throat. The ventilator, sometimes called the “vent,” is a breathing machine that pumps oxygen into the body through a small cannula inserted into the trach. Some patients have a trach but do not require the support of a ventilator.
Will I be able to eat or talk?
Vents do require special attention when it comes to eating. Some people may have trouble swallowing due to the trach or other medical conditions, and will require feeding tubes or special diets of softened foods or thickened liquids.
Speech can present some challenges for people with trachs and vents. While you may be able to learn to use a speaking valve, other options include having your lips read, using a letter board, or writing messages using paper or a whiteboard. Specially trained speech therapists can help you strengthen muscles and find the best way for you to communicate, and can even help you find the best way to get nutrition, whether through oral feeding or other means.
Will I have to live in a hospital?
For many people living with vents, life at home supported by family or home care is not only possible, but optimal. In our experience, some patients can be weaned off of the ventilator entirely through a program of rehabilitation. For other patients, rehab allows them to live independent and active lives. Ventilator programs such as ours at Hillcrest Commons can provide the care you need, whether that’s short-term rehab and education to help you return home and live independently, or long term care with activities and amenities to make sure your new normal is as comfortable and enjoyable as possible.
How can a Speech Therapist help?
Did you know that speech therapists can help with more than just speech? With a thorough knowledge of muscles in the mouth and throat, speech therapists are instrumental in helping vent and trach patients regain strength and improve quality of life. Rehab plans often include a speech therapist who works with patients to retrain and strengthen the muscles necessary in swallowing and speech.
For example, speech therapists can help patients who have difficulty swallowing. They assist in determining the best diet or feeding option for patients with trachs and vents. Bedside swallow exams allow a speech therapist to evaluate a patient’s current abilities, modifying their diet accordingly.
Speech therapists also help patients find the best way to communicate. Vocalizing can be frustrating and tiring with a vent. Goals of therapy may include training to use a speaking valve, strengthening throat muscles to make speech easier, or learning to communicate through non-vocal means.
How is Hillcrest Commons’ ventilator care different?
Our dedicated pulmonary ventilator unit includes an interdisciplinary team of dedicated respiratory therapists and nursing staff with decades of experience. We take pulmonary rehab to another level, with the resources and expertise to care for patients with tracheostomies (trachs) and ventilators (vents). We’re the only program of its kind between Springfield and New York.
Experienced respiratory therapists are available around the clock to provide trach and vent care whenever you need it. Our team also maintains close relationships with five local pulmonologists, ensuring continuity of care for patients transitioning between the hospital, our unit, and home. All of our staff are specially trained to handle ventilators and tubes, helping put you or your loved one at ease.
The unit itself is designed uniquely with comfort and safety in mind. An integrated alarm system immediately notifies nurses and therapists when patients need attention.
The Hillcrest Commons approach to ventilator care:
We recognize that getting off the vent isn’t always the first priority, but it is our long-term goal whenever possible. While other programs may try to wean prematurely, we focus on our patients’ strength and endurance to ensure success. In our experience, a well-developed care routine builds trust with patients and their families, allowing us to share the benefits of our expertise.
Remaining as active as possible also facilitates rehab and recovery. A respiratory therapist joins our recreation staff, ensuring that ventilator patients are able to safely and confidently participate in activities and outings outside of the unit. We are dedicated to quality of life, encouraging patients to get out of bed, eat, and live as independently as possible.
Contact us to learn more about specialized ventilator care at Hillcrest Commons Nursing & Rehabilitation Center in Pittsfield, Massachusetts.